INTRODUCTION
Dr Hussein performs a technique known as: Full-Field subcision under tumescent anaesthesia (Taylor Liberator Technique)
He acquired the technique from Dr Mark Taylor in Salt Lake City USA. Dr Mark Taylor first developed this technique. Currently Dr Hussein is the only doctor in the UK capable of offering this technique.
Patient Suitability
Dr Hussein will have assessed your acne scarring type at consultation. If he feels subcision may be appropriate then he will discuss this technique with you. This tends to be suitable where there are scars that are tethered to deeper layers below the skin. This tethering requires separation using a procedure called subcision. Subcising tethered acne scars allows the depressed scars to ‘pop out’ and the skin will as a result appear less dented.
Quick Links
PROCEDURE DETAILS
Male clients must shave a day before the procedure. Any beards must be removed to allow good visibility of the area to be treated. Hair must be tied back and headbands applied.
Make up must be removed thoroughly.
The skin will be prepared for surgery with Chlorhexidine.
The entire procedure will be performed with the patient lying flat. If there are issues with lying flat for approximately 1 hour then Dr Hussein must be notified pre procedure.
A dermal marker will then be used to mark the acne scars. This is very important as once high- volume tumescent anaesthesia is administered the subsequent tissue deformation can make landmarks difficult to appreciate.
Individual acne scars can also be marked under tangential illumination and it is also useful to delineate the gross affected area. This facilitates a more targeted subcision without the need to unnecessarily subcise unmarked areas which could result in needless risk to various important structures.
The tumescent solution will now be administered using 20ml syringes and 23G needles. Sometimes DrH may use to use a Klein infiltration pump, giving set and a 22G blunt cannula. As the recommended pumps have a high flow rate rapid infiltration can be achieved. This is useful for the technique. Rapid infiltration allows the tissues of the subcutis to become turgid with tumescent mix. This separates the underside of the dermis away from important neurovascular structures. Creating this gap dramatically increases the safety of subcision and reduces the risk of nerve damage and vessel disruption/haematoma. Both sides of the face are infiltrated. There will be a 30 minute wait following initial tumescent administration after which a ‘top up’ of tumescent will be given.
A small puncture incision is made with No.15 scalpel blade and the Taylor Liberator subcision probe can be passed under the skin with relative ease. The forked tip allows for scar bands to be directed towards the blade element of the probe. During passage of the probe under the skin elements of resistance will be encountered. The patient should not feel any discomfort but will feel movement within their cheeks.
Following completion of the subcision the probes will be removed. The entry site is of a small enough diameter (3-4mm) and not under significant tension hence a suture (stitch) is unnecessary.
The skin will be cleaned and dressings applied over the entry site wounds. The patient will be then asked to apply pressure using gauze pads over the treated area for a further 30-minute period. The patient will be observed for a total of 20-30mins after the procedure. If all is well, the patient will be discharged and appropriate follow-up arranged.
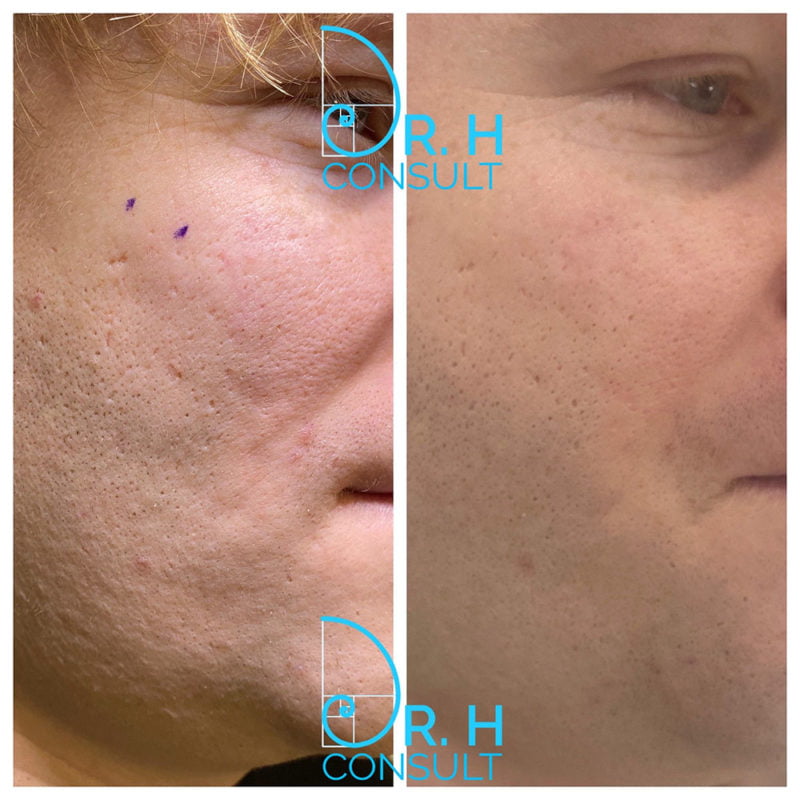
BEFORE & AFTER PHOTOS
POTENTIAL COMPLICATIONS
Surgical Subcision for Scars
Please view below a copy of the Consent Form that you would be required to sign before undergoing this treatment:
What is surgical subcision?
This is a surgical procedure that is designed to free the tethering fibrous scar bands that pull scars inwards and cause indentation and dimpling of the skin. Subcision is performed with a small dissecting probe that is directed by the surgeon toward the underside of the deeper layer of skin (dermis) to release the scar bands. The probe is introduced into this layer by a small linear incision on the facial skin that is 3-4 mm in size. This should heal spontaneously with minimal scarring. The procedure can be performed on almost all areas of the face (excluding the nose and area around the eye) that are dimpled and depressed by scar bands underneath the skin.
What are the benefits of subcision?
Taylor Liberator Subcision fully releases scar bands allowing indented skin to be released and gives skin a smoother appearance.
How is the procedure performed?
Subcision is performed using a dilute mixture of anaesthetic (tumescent anaesthetic) that is injected under the area to be treated. The probe is introduced into the skin and slides along the bottom of the dermis cutting through scar bands that connect the skin to the deeper tissues below.
What are the risks of subcision?
The risks of subcision are similar to other facial surgical procedures and include:
- Bleeding
- Haematoma (collection of blood under the skin)
- Infection
- Scarring
- Temporary or permanent nerve damage
- Swelling or lump from haematoma (blood clot)
- Abnormal skin colour
- Failure to achieve the desired result
- prolonged low grade swelling of subcutaneous fat
Further Information
Nerve Damage
Nerve damage is a potential consequence of subcision treatment. This type of nerve damage has two types of consequence. The first is sensory disturbance to the skin with patches of altered sensation or numb patches.
The second and more severe consequence is disruption to the facial nerve resulting in partial or complete paralysis of one side of the face.
Although the chances of this are quite low due to the level in the skin at which the subcision takes place it is a foreseeable complication of the procedure.
The numbing injection can temporarily reduce movements and mimic paralysis but this movement will return within 24hrs as the numbing injections wear off.
Bleeding
Subcision will inevitably cause some damage to perforator vessels that supply the skin with blood. Bleeding is minimized with the use of a special anaesthetic mix that reduces bleeding from disrupted vessels. It is however possible for a haematoma (clot) to form below the cheek. Small amounts of clot are acceptable and will result in visible bruising. In the worse case scenario a large clot causing pressure or gross facial asymmetry may require surgical drainage.
You will be monitored for a period of 20-30mins post procedure before being able to leave the clinic.
Infection
Your Doctor may give you antibiotic tablets for a period of a week after the procedure to minimize any infection risk. Developing infection will manifest as painful swelling and heat in the affected area after the treatment. If worsening pain and swelling is encountered after the treatment contact Dr Hussein immediately.
Swelling post procedure
Swelling recovery speed is proportional to the amount of bleeding experienced after the procedure is complete.
The greater the bleeding and larger the collection – the longer it takes to resolve. In my practice if I see a large clot/ haematoma I drain it.
Patients in my opinion have an expectation that somehow swelling will resolve quickly within days to weeks. Anaesthetic and bruise swelling settles quickly. Mild soft tissue swelling from Taylor liberator can take up to 6 months or in rare cases a year to settle. But this is low grade swelling confirmed to be soft tissue swelling from surgical subcision trauma on ultrasound.
Numerous ultrasounds many months down the line have shown in the case of mild residual swelling that the cause is simply soft tissue swelling and post-surgical changes. There are no longterm nodules or cysts. Soft tissue swelling is more speedily reduced with diluted triamcinolone steroid injection.
At present although a technical risk we have never incurred motor nerve injury during our liberator procedures. Temporary Sensory loss is not so important – it generally settles by 3 months and no longterm functional deficit is seen.
it is important to expect mild shape change in the cheek – this is because the hypodermis was originally welded to the SMAS layer overlying the muscle causing tethered scarring. Release of the scars will result in slight conformational change of the cheek. This is to be exepected. Remember post liberator the cheek is now in its more natural state – not what you remember your scarred cheek to be like.
If these issues are not encountered post subcision then it is highly unlikely that effective subcision has taken place. This is why blunt cannula subcision recovery is quick. Basically minimal or no effective subcision has been performed
Anaesthetic
Anaesthetic complications – These are exceptionally rare but can include cardiac arrythmia (irregular heartbeat) and cardiac arrest. Anaphylaxis is a possibility (extreme allergic reaction). It is important to understand that technically anaphylaxis, cardiac arrest, stroke, hypoxia and brain damage are all known complications of anaesthetic drugs and sedation. Technically they could occur with any medical procedure performed under general or local anaesthesia with sedation.
It is normal to experience a sensation of stronger and faster heart beating as the anaesthetic mixture injected contains adrenaline. Fine trembling will also be experienced.. You may be drowsy due to sedation. If you have sedation, you must not drive within the first 24 hours following the procedure
Informed Consent
I understand the subcision procedure and all of my questions regarding benefits, risks, costs and alternative treatment including no treatment have been answered. I hereby give consent for the subcision procedure to be performed on myself (or legal dependent).
AFTERCARE
The tumescent anaesthesia used in full field Taylor Liberator subcision causes swelling of the face. This swelling has largely resolved 24-48 hours after the procedure. Facial movements should return slowly following the procedure. A full range of facial motion should be seen on the morning after the procedure. If this is not the case make sure you contact Dr Hussein.
The following precautions should be taken after the procedure:
- No vigorous exercise for 1 week after the procedure
- Avoid any blood thinning medication such as ibuprofen and aspirin for 72hrs post procedure.
- Avoid hot (temperature hot) food and drink for the first 24 hours post procedure.
- Keep the dressings on the entry site wounds on for 24 hours. Change if necessary.
- Do not put pressure, tension or vigorously wash the face for 1 week post procedure.
GOOGLE REVIEWS
1 CO2 laser in which I was supported the whole way through sending daily pictures and advice and feedback daily. Being sent home with every drug that may be needed depending on the how my skin would react after the procedure. If your thinking of CO2 let me tell you it literally knocked 10 years of me I felt totally cared for and in safe hands knowing he was always there no matter what time of day
2. Vascular laser to sort out my rosacea I don’t think I can remember a time in all my life I’ve had such beautiful flawless skin. I’ve always had high colour that’s completely disappeared now, just a beautiful pale complexion
3. Scar maintenance. After having a brow lift I was left ( which is the normal now ) 2 small scar’s just above my brow. Day 10 after surgery he wizzed over the scars with a laser to soften them up so I could get to work on massaging them, and week 12 after surgery he went over with another laser. If I told you 3 months after surgery that they have nearly disappeared I’m not exaggerating. I was advised 6-9-12 months before they would fade. Anything I ever need to have done to my skin, he is my go to. You definitely won’t be disappointed, especially if you’re looking for an outcome that you might think it’s unachievable. Thank you Dr H for always doing what I never thought was possible
Sarah age 58
Only after I found Dr H and had my scars treated by him I got results that I still can’t get used to every time I look in the mirror.
Dr H is truly passionate about what he does and I’m so happy I trusted him as I know some of these procedures may look a bit scary.
I felt extremely well looked after by dr H and his team. After having fully ablative laser done I would send a selfie to drH every day so that he could monitor the healing process and he has always been just a message away which put me at ease throughout the whole process.
I am Fitzpatrick 2 skin type with tethered rolling acne scarring. My scars haven’t completely disappeared but a degree of improvement we have achieved is over 70% which I’m so so happy with.
I can honestly 100% recommend Dr H and his amazing team if you’re struggling with acne scarring. I wish I’d found him sooner as not only I got improvement in my skin but it also has had a positive impact on my mental well-being. I highly recommend dr H and his clinic.
The results have been amazing and exactly what he predicted. From the beginning, he thoroughly explained all options, potential outcomes and ensured I was comfortable with the plan. Unlike others in London, he is not there to just take your money for no results.
He has been absolutely amazing to work with and I cannot recommend Dr H highly enough. He’s very knowledgable and has all the lasers you can imagine - and I’d trust his advice with every single one of them!
Debbie his receptionist is also amazing - she is very kind and accommodating!
I am absolutely satisfied with the result!
I already had a standard subcision in Germany but unfortunately I haven’t recognised any progress.
I am sure that people who suffer from acne scars understand my feelings of a “suddenly whole new attitude to life”.
In winter I will travel again to Dr. H for a full ablative laser treatment and I am really looking forward to meet Dr. H and his amazing team again! Thanks a lot again for that great experience!
I would not hesitate to return, Thank you so much Dr H x
I can honestly say the treatment was completely painless, most of the swelling has subsided this morning, now looking forward to seeing the results in the coming weeks and to have the co2 laser at the end of the year.
A huge thank you Dr H and his team, the service provided from start to finish was amazing.
In terms of the procedures themselves - I had Taylor Liberator Subcision in Nov 2021 & CO2 laser in Jan 2022; I really liked how upfront & direct Dr H was - no hidden costs or additional procedures required - you will be told how it is from day one. The recovery for the laser can be tough, however it’s just a few days downtime for a lifetime of feeling confident & having beautiful skin! So it’s 1000% worth it. Dr H’s aftercare is also second to none - you can contact him directly for any aftercare concerns/questions & you are monitored daily for 2weeks post laser, which really put my mind at ease. Dr H’s assistants who work at the clinic are also really lovely - they both put my mind at rest when I was nervously waiting, pre-procedures.
Overall, I am so so happy that I found Dr H - I only wish I’d discovered him sooner. I will say this; Coming from experience - do not waste your time & money on expensive procedures that will give you a mere 5% improvement (if that) - just see Dr H & get the issue sorted, once & for all! He’s truly the best.
I had taylor liberator subcision and then two treatments of CO2 laser and the results have been amazing, I would say I have seen around an 80-90% reduction in my scarring.
Dr H is extremely thorough and knowledgeable in this field, you instantly feel at ease and assured that he will gain the results he promises.
Although it is more expensive in comparison to other treatments, the results make it so worthwhile.
In terms of the procedure, it looks more scary than it feels! It just felt like a pinch when getting injected and you can’t feel the rest. The recovery time is quick.
I loved the time he dedicated to talk things through with me and the preventative measures he used, as well as his very personal approach before, during and after the procedure. It was extremely re-assuring to have easy access, particularly in the days and weeks following the procedure. I have just had my 4 month post procedure review abs and very happy with the results
Dr H has been available daily with encouragement and advice, I am so happy that I trusted in him, for me it’s the best thing I could have done and I will never be able to thank him enough for the difference he has made giving me confidence in my appearance and now I know longer need to avoid looking at myself.
Save your precious time, money and protect yourself. I really hope people are careful with him because he promises results and fails to deliver. He claims he’s the best in the UK and is very arrogant but yet can’t deliver results. He also claims that he is the only one in UK who does fully ablative laser on his website but there are many dermatologists who does the same treatment so he's not telling the truth. Stay safe everyone!
Before Dr H's amazing procedure I viewed skincare products as a method to camouflage my flaws, not as tool to enhance my appearance. A month has gone by and already my skin feels " baby smooth"!
Still have some redness and dryness to contend with at this stage, but Dr H's WhatsApp facility available to you post procedure, any concerns or queries can be dealt with - it has been an invaluable asset.
I so thankful for the care and attention I have received.
Very unprofessional
I had a fully ablative CO2 laser 3 months ago and it has changed my skin dramatically. I used to have a lot of acne scars and large pores, which at this point are significantly improved (about 50-60%) and the overall appearance of my skin is much healthier than before. The procedure itself is a bit painful but it’s totally worth it. First 3 days of the recovery were the worst part for me personally as I was very exhausted and my face was very swollen. From day 4 onwards I was gradually getting better and by day 8 I had my face fully peeled off, tough it may take a bit longer for some people. From week 2 till week 5 I’ve had hyperpigmentation which was very annoying but it has settled down at week 6. Currently, I still have a bit of pigmentation on my cheeks but it’s easy to camouflage it with a medical grade foundation. For those of you who are still unsure weather or not to go ahead with that procedure I would strongly recommend you to get in touch with doctor Hussein, you won’t regret it!
ETA: It has been a long time since this procedure now and if anything the destruction that he caused has only gotten worse as time goes by.
I had a fully ablative laser with him and my scars almost disappeared specially those on cheeks, some left (beside eyes) but are definitely better.
I tried 3 different dermatologist over a period of THREE years but did NOT got even 10% of what I've got with Dr H, taking my money and time into consideration
In my opinion, DO NOT waste you money and time if you suffer from such a problems just go there and got it sorted.
Good luck
Waited for over a year for my appointment and was cancelled without any notice or even an apology.
Staff are disgustingly rude and have no manners whatsoever.
Used to admire Dr Asifs work but it looks like the success has got to his head which is a real shame.
Money and precious time will be taken from you so please do not fall for this scam.
Stay safe lovely people.

Just wish I was referred to him earlier in my journey.

I am lost for words to say how grateful I am for the incredibly precise work he has done. Last time I saw my skin looking like this I was 13 years old!
He is very friendly and an absolute professional and perfectionist! He supervised the healing process day by day and was very responsive to messages, which made me feel very secure.
Every time I see my face in the mirror I am bursting with joy and I am only 2 weeks post treatment! Dr Hussein gave me back my confidence and I will never be able to thank him enough for the way he's changed my life!



Recently, he has done my CO2 laser resurfacing and I am extremely happy with the outcome. Skin feels a lot smoother to the touch, some old acne scars are gone completely and those that haven't have been significantly reduced, eyelids are less droopy and small under eye wrinkles are gone.



The level of professionalism and customer service that Dr H provides is second to none and I would like to extend that compliment to all the staff there that meet and greet you and make you feel welcomed as soon as you walk in. An all round excellent service that cannot be faulted or recommended highly enough. Thank you, Daniel.




Staff were very welcoming on arrival I was numbed with cream and then injections. The procedure lasted around 40 minutes mostly pain free some areas around my jaw were a bit sore but manageable as Dr H was very reassuring throughout. Most painful part I would say immediately after for around 45mins, I would say your almost in shock but that does go then it’s a very sunburnt feeling and very swollen.
Recovery is lengthy but for results we are after i would say it will be worth it in the end. Im still in recovery atm but it gets better every day. My recovery had been complicated by pseudomonas but managed quickly and effectively by Dr H, he always available through WhatsApp and prescribed what I needed straight away and got it under control.
I do have texture issues and indentation marks and probably massage Him everyday checking that it’s normal, But it is very early days and Dr H has assured me this will all go. I’m very excited to see the end result over next few months.
I will happily come back for 6 months photos Too, thanks Dr Hassien.

But was finally diagnosed correctly by dr h, he prescribed medication which has finally stopped the acne. I have scaring however rather than suggesting expensive treatment which does not work he reassured me it would clear in time. I have not given him 5 stars because I’m too scared too just in case the acne returns however he really does deserve 5⭐️

Day of the procedure
The staff at skin were as welcoming and wonderful as the first time I met them, the lovely lady who works alongside Dr h came and applied my numbing cream and put me at ease, after about a 40 minute numbing wait the lady brought me into the room where I was to have my treatment, Dr h was extremely reassuring the whole time, asking if I was comfortable, explaining everything he was doing and was even kind enough after my treatment to explain everything to my partner, since I was drowsy and tired ( please have someone to escort you home) he gave me his contact number to monitor me throughout my recovery.
Following days after treatment
Next day
My face swole as expected eyes super tight and puffy the following day, it was a little scary due to the fact I couldn't see too well, (this is completely normal and to be expected though)
Am and pm routine for 10 days
Wash with dermol apply Vaseline or aquaphor
Meds
Update Dr h with selfies
By day 2 yellow oozing and crusts were on my face (which is a good sign) and this continued for a couple of days, Dr h assured me everyday that things were going well I was healing as I should be
By day 3 all major swelling was gone and eyes looked all youthful and bright - outstanding! Skin was still peeling and gross though
Day 4-7 still around the clock aftercare and support from Dr h via calls and Watts app, things were vastly improving, any questions I had were answered promptly, Dr H was extremely supportive!
(Overall mood from day of treatment to day 4 was eat sleep and repeat lol. Plenty of high calorie snacks and fluid)
Day 7-10 fucibet cream was to be applied for 3 days am and pm followed by my Vaseline
Day 10 - today using gentle face wash and moisturising cream by a brand called ceraVe and spf 50+, skin looks brand new, little bit of rough texture on cheeks which is common after resurfacing and will always settle in a few weeks, I am looking forward to seeing my full results in 3-6 months, I don't want to speak too soon but I don't have a visible imperfection on my face! Dr h is the only person who will be performing any future treatments I may ever need later down the line in regards to laser. I have passed on his information to my sister and mother who will no doubt be in touch with him soon! Many thanks Dr H and team!

I will start by saying that I'm probably not the most obvious candidate for it as I'm only 30 and have been fortunate enough not to suffer acne scarring however I am a skin obsessive and perfectionist so I see a thousand flaws and I had it done as I wanted to get rid of some of the fine lines that had taken up residence over the last 5 years or so as well as other imperfections.
The procedure itself wasn't painful (at least not most of the time) and Dr H was very reassuring however it does leave you feeling rather in shock afterwards I found, so if you can, have someone waiting for you after. I was prepared for pain in the immediate recovery days what I wasn't prepared for was how little I would be able to see due to the swelling up around my eyes (audio books are your friend at this point people! Also plenty of painkillers and food that you can eat without having to open your mouth too wide because that will hurt too.)
I had a week off from work and then I had to go back and well looking at me was definitely pretty shocking - no longer hideous like I had been (there is a definite hideous monster stage of recover, no point sugar coating it) but pretty darn shocking. I had a lot of odd looks and as a teacher I gave my poor kids a bit of a shock but thankfully kids are super accepting. Every time I caught a glance of myself in the mirror though I'd be like "wow the kids are amazing!" they treated me just like normal after the initial morning of shock wore off and honestly I looked pretty awful for a while. Kids are way better at that stuff than adults.
You just have to roll with it and concentrate on making sure you're doing everything right to help your skin recover. I didn't rush to put make-up back on or anything because honestly why potentially mess something so major up by not just waiting a little while longer. I did unfortunately get an infection around my eyes which meant they took longer to heal overall but Dr H soon got the infection itself cleared up and he checked the selfies daily. The recovery can be hard, I expect some people heal a lot more quickly than I do but I'm not a fast healer and it isn't easy to constantly have to put yourself out there not looking like yourself. It was at least month before I started feeling like my outside reflected my inside again and it can make various aspects of life difficult.
Shortly before lockdown happened in the last week of schools being open I was wearing very light make-up again and looking passably normal but although probably not noticeable to most people I was pinker in overall tone and that takes a long time to fade. I was finally feeling attractive again though - yay! I think my skin appreciated lockdown and having more time of zero commute/pollution/little make-up as it gave it more recovery time and I now look totally normal.
Well I say normal...I look better! The little lines around my eyes - gone! My cheeks - plumper! Gotta love that collagen. My mum says my cheeks remind her more of 19 year old me. It has also slightly softened the frown between my eyebrows (that thing is a curse) It hasn't totally perfected my skin but it has done a darn good job of all but the most problematic area of it. My friends say I look really good and I did not look bad before! It is quite fascinating because it is basically impossible for someone to put their finger on exactly what is different but something subtle is.
I think if you had more skin irregularities or older skin you would probably see more dramatic results but it would still be very natural looking. I would have it or something similar done again in another 10 years or when I felt it needed doing but I urge you do plan enough down time! Was it worth it? Yes..but I'm not rushing to go through that recovery again 😉
I hope this has been helpful 🙂 Thanks Dr Hussein 🙂









I had very large pores and sun damage on my skin, I had halo laser but it was a light laser for the size of my pores so we attempted a mild Co2 laser, today is day 11 and I can't be happier with the results, the large pores have reduced a lot! My skin looks younger, healthier, still a bit red but that will settle soon.
I have definitely achieve what I wanted I am not going to wear make up foundation for a while ????.
Dr H has been there for me every time I had a question, daily since the first day giving me advice and looking after me.
It was the best money investment I've done on my skin.
Also mention Iulia, she has been incredible taking care of me while I had the treatment as I had to go on my own to the clinic, reassuring me and making sure I was fine.
I know how important is this as I am a nurse myself, they both made me feel like at home.
Thank you all! ????????


He definitely knows what he does!
I can already see big improvement on my skin texture even though I know my skin still needs loads of time to fully settle so the improvement will continue.
Thank you